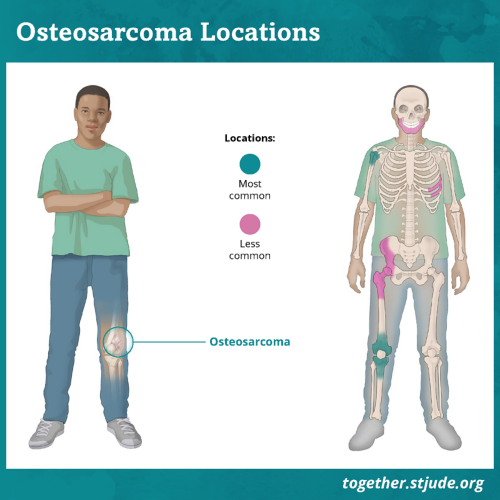
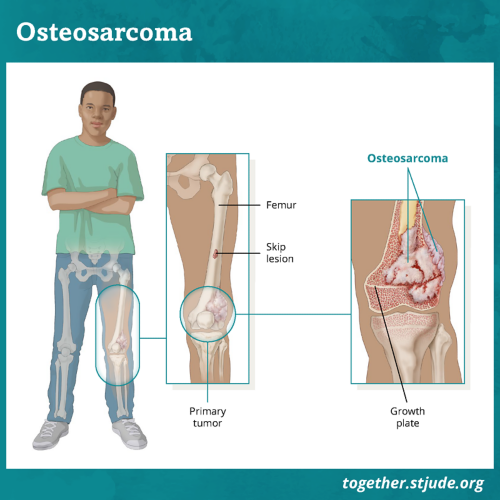
Osteosarcoma may develop in any bone. But it usually forms in the wide ends of long bones of the leg or arm. It most often begins in immature bone cells that form new bone tissue.
The most common places for osteosarcoma to develop are in the:
- Lower part of the thigh bone near the knee
- Upper part of the shin
- Upper arm bone near the shoulder
It sometimes forms in flat bones such as the pelvis or skull.
In rare cases, osteosarcoma can form in soft tissue other than bone.
Osteosarcomas may form inside the bone or on the outer surface of bone. Most pediatric osteosarcomas are inside the bone.
Osteosarcoma is usually treated with chemotherapy followed by surgery.
Children with a single site of osteosarcoma that can be removed with surgery have a 65–70% chance of long-term cure. Survival rates are lower if the cancer has spread at the time of diagnosis.
Symptoms of osteosarcoma
Osteosarcoma damages and weakens the bone. Symptoms depend on where the tumor is located. They may be hard to notice at first. They can also be like symptoms of other conditions.
Symptoms of osteosarcoma include:
- Pain in a bone or joint
- Problems moving the joint
- A lump or swelling over a bone
- Limping or problems walking
- A bone that breaks
Pain may worsen over weeks or months. The pain may cause your child to wake up in the middle of the night.
Over-the-counter pain medicines such as ibuprofen or acetaminophen may not relieve pain over time.
Risk factors for osteosarcoma
Osteosarcoma typically develops after age 10. It is rare before the age of 5.
These factors may increase risk for osteosarcoma:
- Osteosarcoma is slightly more common in males than females.
- Black children have a higher risk of osteosarcoma than white children.
- Cancer survivors who were treated with radiation therapy have a higher risk for developing osteosarcoma.
- Genetic factors may increase risk for osteosarcoma. A small number of children have changes in genes that put them at higher risk for some cancers. People at a higher risk include those with:
- Retinoblastoma that is passed down through families
- A history of multiple cancers
- A strong family history of
- Other rare, conditions that are passed through families may also increase risk for osteosarcoma. These include:
Diagnosis of osteosarcoma
Several tests are used to diagnose osteosarcoma. They include:
- Health history and physical exam
- Blood tests to learn about symptoms, general health, past illnesses, and risk factors.
- Imaging tests to look for tumors and help determine other tests that are needed.
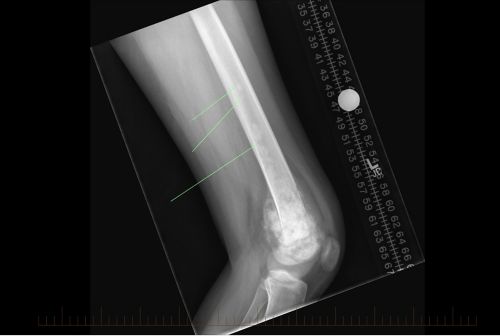
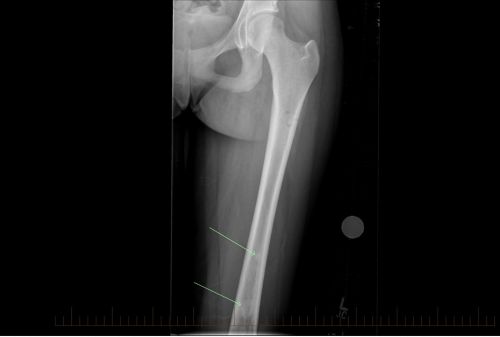
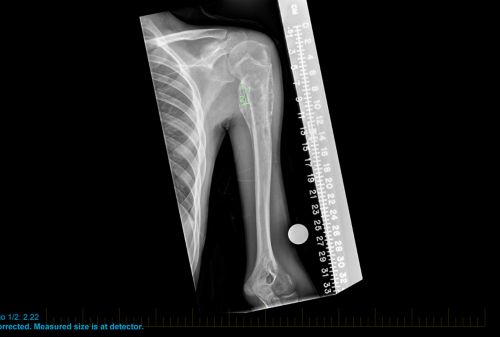
- An x-ray to see if osteosarcoma has spread to other parts of the bone.
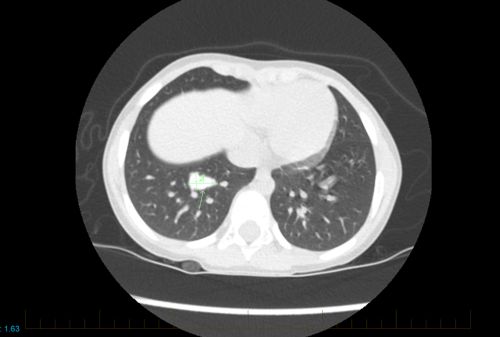
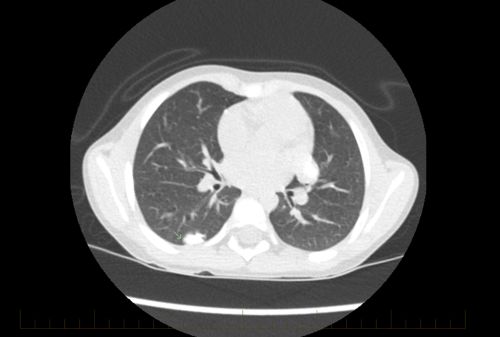
- A CT scan of the chest to see if osteosarcoma has spread to the lungs.
- An MRI is used to assess the tumor and assist in planning surgery.
- Full body imaging using bone scans or PET scans to look for spread of osteosarcoma to other areas of bone.
- A biopsy. In a biopsy, the doctor removes a small amount of tissue from the tumor. Doctors will look at the cells with a microscope to find signs of cancer.
Staging of osteosarcoma
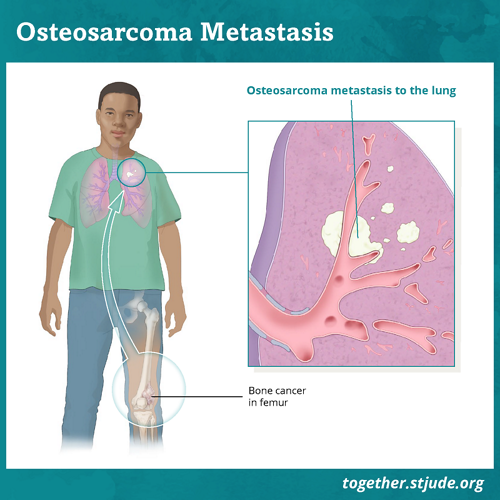
Osteosarcoma is usually described as either localized or metastatic.
- Localized osteosarcoma means that there is a tumor in only 1 place.
- Metastatic osteosarcoma means that the cancer has spread to other places.
Treatment of osteosarcoma
Osteosarcoma is usually treated with chemotherapy followed by surgery.
Other treatments such as radiation therapy may be needed if the tumor cannot be removed or if any disease is left behind after surgery.
Prognosis for osteosarcoma
Prognosis depends on several factors:
- Whether the cancer has spread to other parts of the body
- The ability of surgery to completely remove the tumor
- Response of the tumor to chemotherapy
- If the cancer has come back
Patients with a single, localized osteosarcoma that can be completely removed with surgery have a 65–70% chance of long-term cure.
If osteosarcoma has already spread at diagnosis, the chance of survival is about 30%.
About 30% of patients will have cancer that comes back. This most often occurs in the lungs.
For those who relapse, prognosis depends on factors such as:
- The ability to remove the tumor
- When relapse occurs. Cancer that returns within 18 months of diagnosis is usually more difficult to treat than cancer that returns later.
If cancer is treated and comes back, the 10-year survival rate is about 17%. Advances in therapies are continuing to help some children.
Talk to your care team about problems to expect and ways to help manage them. Palliative care can help you manage symptoms, promote quality of life, and make informed decisions.
Life after osteosarcoma
Monitoring for return of cancer
Your child needs follow-up care every few months to see if cancer has returned. These visits occur for several years after treatment ends.
Screening tests usually include:
- Blood tests
- CT scans of the lungs
- X-rays of the affected bone
Patients with certain inherited syndromes or genetic conditions may be at risk for future cancers. They may need other follow-up care.
Life after limb-sparing surgery or amputation
Most osteosarcoma patients who have amputation or limb-sparing surgery do well over time.
They report good physical function and quality of life. Follow-up care is important.
Your child should have an annual exam to check muscle and bone function. It is important to make sure that there are no ongoing problems. Uneven limb length, changes in the way your child walks, joint issues, or other problems can cause chronic pain or disability.
- If your child had an amputation, they should also have an annual exam to maintain the function of the prosthetic limb.
- An orthopedic surgeon should check your child once a year if they have a bone graft and/or metal implant.
- If your child had limb-sparing surgery, they may need other surgeries for limb lengthening until they reach adult size.
—
Reviewed: December 2022