Renal (kidney) tumors occur when cancer cells form in kidney tissues. These tumors account for about 7% of all childhood cancers.
There are different types of kidney tumors in children. Wilms tumor (nephroblastoma) is one type of childhood kidney tumor.
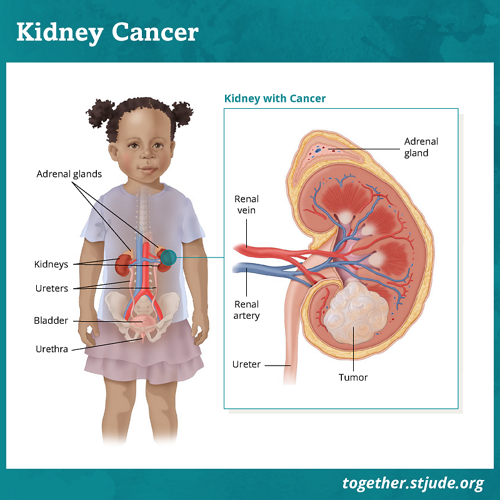
The kidneys are a pair of organs on either side of the spine in the back of the belly. They filter and clean the blood. The kidneys also make urine.
Wilms tumor is also known as nephroblastoma. It is the most common kidney cancer in children. About 500 children in the United States are diagnosed with Wilms tumor each year. It is most often found in children under age 5.
Renal cell carcinoma is the most common kidney tumor in teens between ages 15–19.
Other kidney tumors include:
- Clear cell sarcoma of the kidney
- Malignant rhabdoid tumor
- Mesoblastic nephromas
Sometimes cancer may have spread before diagnosis. This depends on the type of tumor your child has. Wilms tumor, for example, rarely spreads to the brain.
Areas where cancer might spread can include:
- Lungs
- Liver
- Bones
- Lymph nodes
Treatment for most kidney tumors depends on the tumor. It may include:
The treatment and prognosis for kidney tumors depends on the type of tumor and whether it has spread to other organs. Your child’s doctor is the best source of information on your child’s case.
Risk factors for kidney tumors
Certain genetic syndromes or other conditions may increase risk for kidney tumor. But most kidney tumors are not genetic.
Genetic conditions that increase the risk include:
- WAGR syndrome
- Denys-Drash syndrome
- Overgrowth syndromes (such as Beckwith-Wiedemann syndrome)
If your child’s care team thinks your child’s tumor might be caused by a genetic condition, they may suggest genetic testing.
Diagnosis of kidney tumors
Tests to diagnose kidney tumors include:
- The patient’s medical history
- A family health history to find out if the cancer has been passed down through your family.
- A physical exam
- Lab studies to look at blood and urine including:
- Complete blood count
- Liver and kidney tests to find out how the organs are working
- Electrolyte tests to look at levels of sodium, chloride, magnesium, potassium, and calcium
- Urinalysis to test the urine for sugar, protein, blood, and bacteria
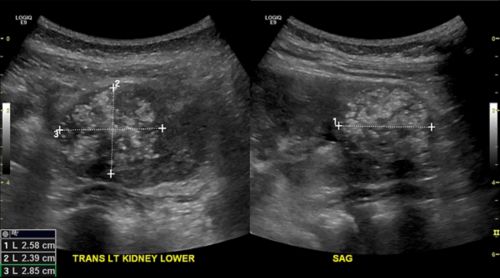
- Imaging of the belly to find out if a tumor is present, see how big it is, and find out if it has spread.
- Examination of tissue that has been taken from the tumor. This will help doctors learn more about the type of cancer. This may be done through a biopsy or after surgical removal of the tumor.
Kidney tumors are classed based on the size of the tumor and whether the cancer has spread. Imaging tests, surgery, and pathology give information for the stage of disease. For all kidney tumor types:
- Stage 1 and Stage 2 disease mean the cancer has not spread outside the kidney.
- Stage 3 disease has spread outside the kidney. But the cancer is still inside the belly.
- Stage 4 disease has spread outside the belly. It can be in the:
- Stage 5 disease (for Wilms tumor only) means both kidneys are affected.
Patients whose cancer has spread to other parts of the body have a poorer prognosis. This is because the cancer is more serious. It is also harder to treat.
Support for patients after kidney cancer
Monitoring for recurrence
Patients will get follow-up care to screen for recurrence after treatment. Your child’s care team will suggest the tests your child needs.
If your child has a syndrome or genetic difference that is passed through families, they may need genetic testing and extra care.
Life after nephrectomy
Patients who have had a kidney removed can lead normal, active lives.
It is important to talk about medical needs and lifestyle habits with your child’s care team.
Your child will need regular medical care with a check-up at least yearly. Tests might include:
- Blood pressure
- Kidney function (BUN, creatine)
- Urinalysis
Your child may need to see a kidney specialist called a nephrologist.
Ways to protect kidney health
- Drink about 6–8 cups of water per day. Stay hydrated when playing sports and in hot weather.
- Limit caffeine.
- Be careful with the use of non-steroidal anti-inflammatory drugs (NSAIDs). These medicines can harm the kidneys when used too often or taken in too high of a dose. Avoid these medicines when possible. Talk with the care team before your child takes them.
- Check with a doctor or pharmacist before taking a new medicine. This includes prescription and over-the-counter medications as well as herbal supplements. Make sure all health care providers and pharmacists know your child has only one kidney.
- Avoid constipation by staying hydrated and eating fiber. Take medicines to soften stool if your child’s care team suggests them.
- Make sure your child is ready before potty training to avoid issues with holding urine.
- Call the doctor at any sign of urinary tract infection (UTI) or kidney infection.
- Be physically active. Most physical activities and sports (including contact sports) pose little to no risk to kidney health. Talk to your child’s care team about activities and any concerns.
Late effects
Children treated for kidney tumors are at risk for late effects related to therapy.
Living a healthy lifestyle, eating a healthy diet, and having regular screenings and checkups can help protect your child’s health.
Survivors treated with systemic chemotherapy or radiation should be monitored for acute and late effects of therapy. Depending on the type of treatment given, these effects can include:
Your child’s doctor is the best source of information about your child’s case.