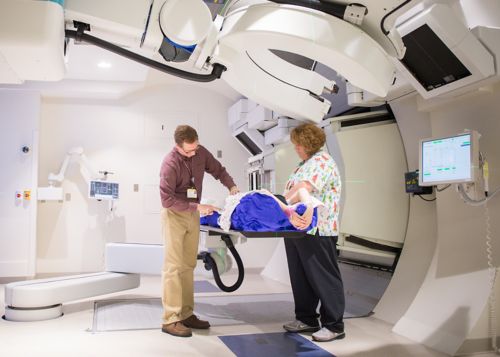
Radiation Therapy for Childhood Cancer
What is radiation therapy?
Radiation therapy (also called radiotherapy) uses either high-energy x-rays (photons) or protons to shrink tumors and kill cancer cells. Radiation damages cancer cells so that they stop growing and dividing.
Sometimes radiation may be the only treatment your child needs. Or radiation may be used with other treatments, such as surgery and chemotherapy.
Radiation targets cancer, but it may affect nearby healthy tissue and cause side effects. Your care team plans treatments for effectiveness and safety.
Types of radiation therapy
Radiation therapy can be given in different ways. Types include:
Benefits of radiation therapy
Radiation therapy can have different goals depending on your child’s diagnosis and treatment plan. It may be used to:
- Target, shrink, and destroy cancer cells
- Make surgery easier or help your child avoid surgery
- Prevent cancer from coming back after other treatments
- Relieve symptoms such as pain, bleeding, or shortness of breath (called palliative radiation therapy)
- Work along with other treatments, like chemotherapy
Before radiation therapy
Consultation
You will meet members of the radiation therapy team. They will explain the treatment process and side effects. They will also answer your questions. It may be helpful to bring someone with you to take notes. If you have more questions after the appointment, you can contact your care team.
Radiation simulation
Radiation simulation is the first step in planning your child's radiation treatment. Your child will have imaging tests done, such as a CT scan or an MRI. This helps your team see where the tumor is (or was) so they know how to position your child for treatment.
The care team will make small marks or tattoos to help position your child for the radiation. They may also make a mask or body mold to help your child lie still in the correct position during treatment.
Treatment planning
The radiation oncologist is the doctor in charge of radiation therapy. They work with the radiation therapy team to develop a treatment plan for your child. The treatment plan will include:
- The total amount of radiation your child will get
- How often your child will get radiation therapy
- Where the radiation will be aimed
Discussing the treatment plan
The radiation oncologist will explain:
- How long each session takes
- How many treatments are needed (often 5 days a week for 1–7 weeks)
- Breaks between treatments
- Why staying still is important
- What side effects to watch for
- A personalized plan for keeping your child safe and comfortable during radiation, which may include:
A child life specialist may help explain radiation therapy to your child in a way they will understand.
What to expect during radiation therapy
Radiation is usually given as an outpatient visit, so your child will not have to stay in the hospital overnight. If anesthesia is needed, your child will have a separate appointment for getting the anesthesia medicine.
Follow your care center’s steps for registration and check-in. During registration you may:
- Check in at the registration desk.
- Go with a staff member to the treatment room.
- Meet the anesthesia team if anesthesia is needed.
Once your child is in the treatment room:
- The team will position your child on the table using the marks, mask, or body mold made during simulation. Positioning usually takes longer than the actual radiation treatment.
- The therapist will leave the room to start treatment. They can see and talk to your child the whole time.
- The radiation therapy machine will line up to target the treatment spot. Your child may see lasers that help with positioning. They will not feel them.
- Your child will not feel or see the radiation. It does not hurt. They may hear a noise from the machine.
Tips to prepare for radiation treatments
- Arrive on time or a few minutes early for appointments. Being late may mean waiting longer.
- If a mask is used during radiation treatment, your child’s hairstyle needs to be the same as it was when the mask was made.
- Have your child wear loose, comfortable clothing such as T-shirts with sweatpants, pajama bottoms, or other elastic waist pants.
- Care centers have different rules about observing therapy sessions. Some let caregivers watch from a nearby room, or you may need to wait in the waiting area. Siblings usually need to stay in a waiting area with an adult, so plan ahead for their care.
If no anesthesia was used, your child can usually return to their usual activities as soon as treatment ends. If anesthesia was used, your child will need time to wake up and recover.
For most types of radiation therapy, there are no restrictions on contact (hugging, touching, caring for a child) after treatment. Your child may return to school and regular activities right after radiation therapy if the care team says it is OK.
If your child gets internal radiation therapy such as MIBG therapy, there will be rules for avoiding close contact with others after treatment. This is especially true for contact with young children and pregnant women. Ask your care team about specific guidelines for your child.
Caring for your child after radiation therapy
Skin care: Skin changes might get worse for 7–10 days after your child’s last radiation treatment. It is important to take good care of the skin during this time.
Eating and drinking: After radiation, your child may not feel as hungry as usual for a few weeks. It is important for your child to eat healthy foods and drink plenty of water. If they have nausea or vomiting, give them their prescribed anti-nausea medicine. Call the care team if the medicine does not help.
Rest and activities: Your child may have low energy for weeks or even months after therapy ends. Their body is working hard to repair itself, so they need plenty of rest.
Follow-up visits
Your child will have regular follow-up visits with the radiation oncologist. This may include diagnostic imaging tests such as CT, PET scans, or MRIs to monitor how well the cancer responds to treatment.
Possible risks of radiation therapy
Radiation therapy can cause side effects, including:
These side effects depend on where the radiation is given. Some can last for weeks or, rarely, months. Most go away with time.
| Location |
Possible Side Effects |
|---|
| Head/Neck |
Fatigue
Hair loss
Nausea and vomiting
Headache
Blurry vision
Mouth changes
Taste changes
Throat changes, such as trouble swallowing
Less active thyroid gland |
| Chest |
Fatigue
Hair loss
Sking changes
Throat changes, such as trouble swallowing
Cough
Shortness of breath |
| Stomach/Abdomen |
Diarrhea
Fatigue
Hair loss
Nausea and vomiting
Sking changes
Urinary and bladder changes |
| Pelvis/Rectum |
Diarrhea
Fatigue
Hair loss
Nausea and vomiting
Sexual problems
Fertility problems
Skin changes
Urinary and bladder changes |
Source: National Cancer Institute
Long-term effects of radiation
Radiation may cause long-term and late effects. These are side effects that show up later in life.
A rare late effect is cancer in the treated area. Regular follow-up visits are important to check for cancer.
When to call your care team
Call your care team right away if your child has:
- Fever or signs of infection
- Red, swollen, or painful skin where they got radiation, especially if it looks infected (warm, oozing, or has blisters)
- Trouble breathing or shortness of breath
- New or worsening pain that does not get better with medicine
- Vomiting or diarrhea that does not stop or keeps your child from eating or drinking
- Trouble swallowing or eating
- Headache, confusion, extreme tiredness, or changes in behavior (like acting very sleepy, irritable, or not responding as usual)
- Any bleeding (nosebleeds, blood in urine or stool, or bleeding from the mouth)
- Signs of dehydration (dry mouth, not peeing much, crying without tears, or sunken eyes)
- Anything that worries you or makes you unsure about your child’s condition
Questions to ask your care team
- Why does my child need radiation therapy?
- What type of radiation therapy will my child get?
- What are the goals of the treatment?
- How does radiation therapy work?
- Are there any alternative treatments?
- What should we expect with radiation therapy?
- Will I be able to stay with my child during treatment?
- What are the risks and side effects of radiation therapy?
- When should we call the care team?
Key points about radiation therapy
- Radiation therapy uses beams or waves of energy to kill cancer cells.
- Radiation simulation is used to help plan your child’s radiation treatment.
- Your child must stay still during treatment. A mask or body mold may help keep your child’s body in the correct position.
- If your child gets general anesthesia, follow all instructions about not eating or drinking before treatments.
- Radiation side effects may include tiredness, skin changes, hair loss in the area, and nausea.
- Ask your care team any questions you have about radiation therapy.
Learn more about radiation therapy
-
Brachytherapy
Brachytherapy uses a tiny radioactive source (sometimes called a seed) placed inside the body to kill tumor cells. It is also known as internal radiation therapy.
-
Radiation Simulation
Radiation simulation is the set-up or planning session to help the care team plan the radiation treatments. Learn what to expect during a simulation visit.
-
Proton Beam Radiation
Proton beam radiation therapy is a type of radiation therapy using protons as its energy source. This therapy allows doctors to aim high doses of radiation at tumors and minimize damage to nearby healthy cells.
-
How to Care for Skin During Radiation Therapy
Radiation therapy can cause skin irritation, including redness, peeling, dryness, and itching. Learn how to care for your child’s skin during radiation therapy.
-
Radiation Therapy Team
The radiation therapy team cares for patients having radiation treatments. The team will explain the treatment process and answer questions.
-
Surface Guided Radiation Therapy (SGRT)
Surface Guided Radiation Therapy (SGRT) uses special cameras and lights to help position your child for radiation treatment. Learn what to expect during SGRT.