Menu
Close
Back
Welcome to
Together is a new resource for anyone affected by pediatric cancer - patients and their parents, family members, and friends.
Learn More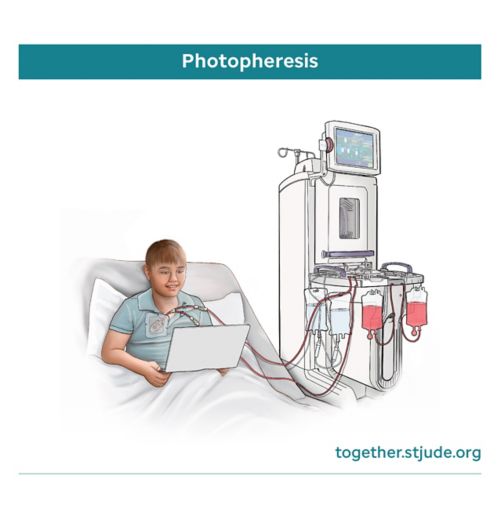
Photopheresis is a type of apheresis that removes white blood cells from the blood and treats them with UV light.
Photopheresis is a procedure that treats white blood cells with ultraviolet (UV) light. It can be used to help treat conditions such as graft versus host disease (GVHD).
Photopheresis is a type of apheresis, a procedure to remove a part of the blood. A machine separates the blood and removes white blood cells. The medicine methoxsalen (Uvadex®) is added to these white blood cells. The white blood cells are exposed to ultraviolet (UV) light. This activates the medicine. After white blood cells are treated, they are returned to the body with the rest of the blood. Only a small part of your child’s blood is out of the body at any time.
The UV light from photopheresis changes how white blood cells work. White blood cells are part of the body’s immune system. By treating white blood cells, photopheresis helps to regulate the body’s immune system.
The night before and the day of the procedure, your child should avoid eating high-fat foods. If there is too much fat in the blood, the machine may not be able to separate the blood cells and the procedure may need to be stopped early.
The process of photopheresis can take 2 to 4 hours. Your care team will explain what to expect and answer any questions.
Your child will be in bed during the procedure. Have your child wear comfortable, loose-fitting clothing. During the procedure, your child can watch a movie, read, color, or have games or toys that can be played with in the bed.
Your care team decides the best way to access your child’s veins based on the size of their veins and the number of times they may have photopheresis treatments. The procedure is usually done with 2 lines (double needle procedure). Types of access include:
Your child’s care team may need to give your child fluids along with the blood that is returned to them. The fluid may be a saline solution. Or it may be saline mixed with albumin. Albumin is a purified blood protein. In some cases, your child may need a blood transfusion.
Your provider may give your child a medicine called heparin. It is a blood-thinning medicine. It keeps the blood from clotting in the apheresis machine.
Your care team will take steps to reduce the risk of infection. All tubes that touch the blood are sterile (free from germs) and are only used once.
An apheresis nurse will stay at the bedside to monitor for any reactions or problems.
Because your child will have tubes attached to the apheresis machine, they will not be able to leave the room once the procedure has started. Portable toilet equipment will be provided if needed.
The side effects of photopheresis are similar to those that can happen when someone donates whole blood. Any side effects are usually mild and temporary. There is always the risk of rare or unknown side effects.
Side effects may include:
Some people have a decrease in blood pressure after the procedure. This can cause your child to feel dizzy or lightheaded. If this happens, have your child sit or lie down and raise their legs slightly. Give cool liquids to drink when they feel better.
Methoxsalen makes your child’s skin much more sensitive to the sun. For at least 1 day after the photopheresis procedure take steps to protect your child’s skin and eyes.
Your child should:
During photopheresis, your provider may give your child a medicine called heparin. This is a blood-thinning medicine. It keeps the blood from clotting in the machine.
Heparin may cause side effects that include:
Tell a member of your care team right away if your child has any of these symptoms during photopheresis:
If you have questions about your child’s procedure, talk to your care team.
—
Reviewed: December 2023

Your child may need a blood transfusion if they don’t have enough blood cells. Learn about types of blood product transfusions and what to expect.

IV stands for intravenous (inside the vein). An IV is a small tube called a catheter. It is inserted into a vein. The IV is about the size of a small straw or coffee stirrer.

A central line, also known as a central venous catheter, is a thin tube placed into a large vein that leads to the heart. Learn more about central lines.