Hearing loss is a possible side effect of some pediatric cancers or cancer treatments. Certain cancer medicines and other treatments, including radiation and surgery, can damage the ear, resulting in hearing loss. In some cases, hearing loss may develop due to the tumor itself.
Children who receive ototoxic therapies (treatments known to cause ear damage) should have regular hearing tests to watch for problems. Hearing loss can affect speech, social relationships, learning, academic achievement, and career goals. Early assessment and intervention can help patients and families better manage hearing loss to promote quality of life after cancer.
Ways to protect hearing
- Reduce exposure to loud noise.
- Use hearing protection.
- Decrease the volume of personal listening devices.
- Get hearing tested.
- Let the care team know about any changes in hearing.
In some cases, the care team may recommend changes to medicines or other treatments based on hearing loss.
Symptoms of hearing loss in children
- Ringing in the ears
- Having trouble hearing or understanding, especially in crowds or with background noise
- Not paying attention
- Not reacting to sounds
- Turning up the volume of television or music
- Having problems in school, such as not following directions or a drop in grades
- Turning the head to try to hear better or using a “good ear”
- Change or delay in speech
- Balance problems
Find more information on hearing and communication in babies and young children.
Causes of hearing loss
Risk factors for hearing loss in childhood cancer patients include:
- Certain chemotherapy medicines, especially platinum drugs such as cisplatin and carboplatin
- Radiation to the ear, brain, nose, throat, sinuses, or cheekbones
- Surgery affecting the ear, brain, or auditory nerve
- Other medications
- Certain antibiotics such as erythromycin or aminoglycoside antibiotics including amikacin, gentamicin, and tobramycin
- Certain diuretics that work in one area of the kidney including furosemide and ethacrynic acid
- Health factors such as premature birth, low birth weight, or previous infections or illnesses
Receiving treatments at a younger age and/or more intensive dose of chemotherapy or radiation also increases the likelihood of hearing loss.
The ear and hearing
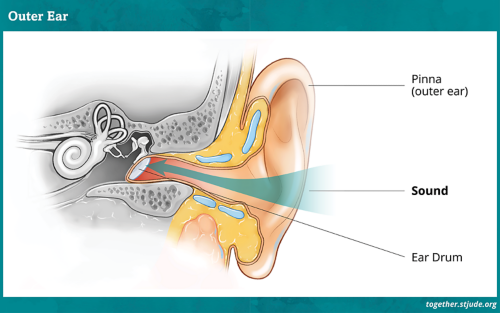
There are three main parts of the ear:
- Outer Ear – Sound waves enter the ear through the outer ear. It acts like a funnel to direct sound to the ear drum, which separates the outer and middle ear.
Types of hearing loss
Different types of hearing loss may be seen childhood cancer patients and survivors. Hearing problems due to chemotherapy are likely to affect both ears. However, hearing loss after surgery or radiation may be in one or both ears, depending on the specific type of damage. For some patients, hearing may improve over time. For many patients, hearing loss is often permanent and may get worse with age. Some survivors may start to have hearing problems months or years after treatment ends. These problems are known as late effects. Understanding the type of hearing loss is important to help in planning care and monitoring.
Conductive Hearing Loss
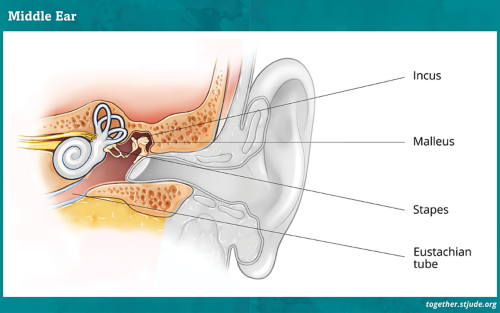
This type of hearing loss when there is blockage or damage in the outer or middle ear. Fluid, wax, or swelling may prevent sound from traveling normally, causing sounds to seem “muffled.” The eardrum or bones of the middle ear may also be stiff or damaged. Infection can be a common cause of conductive hearing loss. Radiation therapy may also cause conductive hearing loss in one or both ears.
Sensorineural Hearing Loss
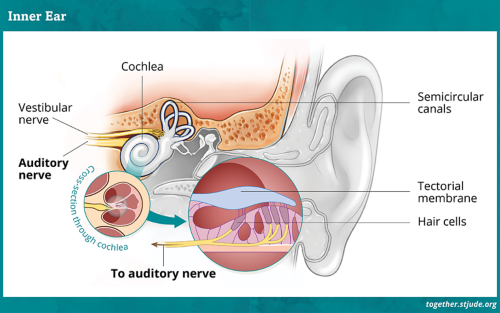
Sensorineural hearing loss results from damage to the hair cells of the inner ear (sensory) or to the auditory nerve or brain (neural).
- Chemotherapy can travel into the fluid of the cochlea where it is absorbed by hair cells. Certain types of chemotherapy medicine harm hair cells. When sensory hair cells are harmed, vibrations reach the hair cells, but they can’t send the sound signals to the brain. Usually, hair cells that transmit high-frequency (high-pitch) sounds are damaged first. If damage continues, ability to hear lower-pitch sounds may worsen.
- Depending on where radiation is delivered, radiation can harm hair cells or damage nerves or parts of the brain that interpret sounds. Children who received doses of radiation higher than 30 gray (Gy) to vulnerable areas are at higher risk.
- Surgery can also cause damage to the nerves or brain areas involved in hearing. Pressure from swelling or a tumor can sometimes keep nerves from working properly.
Hearing loss in pediatric cancer patients may be conductive, sensorineural, or a combination. Conductive hearing loss may improve over time if the cause of the problem, such as fluid or swelling is removed. Sensorineural hearing loss is likely to be permanent, especially if hair cells or nerves have been damaged by chemotherapy or radiation.
Help for hearing loss
Patients at risk for hearing loss should have hearing tested by an audiologist. A common type of hearing test is an audiological evaluation in which the patient listens to different sounds through earphones. The audiologist records what sounds and pitches can be heard for each ear. The results are recorded on an audiogram and compared to the levels expected for normal hearing. This test is also used to monitor hearing over time. Hearing can also be tested by monitoring brain waves in response to sound. This test is called an Auditory Brainstem Response (ABR). Based on risk factors and hearing loss symptoms, the audiologist will recommend follow-up testing and monitoring.
A variety of services and assistive devices are available to help with hearing disorders. These include:
- Hearing Aids – Hearing aids are devices that make sounds louder. Behind-the-ear models are recommended for younger children. They are easier to use and allow for growth. Smaller hearing aids may be a good option for teens and adults. Learn more about hearing aids in children.
- Cochlear Implants – Cochlear implants are surgically implanted devices that stimulate the auditory nerve. However, they do not work for all types of hearing loss.
- Hearing Assistive Technology Systems (HATS) – Also called assistive listening devices, these systems include: frequency modulation (FM) systems, infrared systems, induction loop systems, telephone amplifiers, text telephones, and alerting devices. These systems may be available in public settings (such as schools, churches, or theatres) or for home use. Each system is designed differently, but the goal is to amplify sound or transform sound to a different form such as text. Learn more about hearing assistive technology.
- Additional Communication Methods – Speech reading and sign language can be helpful for people with more severe hearing loss. Sign language interpreters may be available in settings such as schools and hospitals to assist in communication.
An audiologist can help match patients with the best services and devices to fit their needs. It is important that parents make sure that children use their hearing devices properly and keep follow-up appointments to monitor hearing. Hearing loss is associated with problems in different areas including school, work, and relationships. However, being consistent with wearing hearing aids or other devices and using available services (such as Individualized Education Plans – IEP) can help give children the best chance for success in life after cancer.
Tips for patients and families
Know your risk. Talk to your care team about cancer treatments (including dose received) and other risk factors for hearing loss.
Get tested and watch for symptoms. Have a baseline hearing test and get regular monitoring to catch hearing changes early. Symptoms of hearing loss can be easy to miss. Be aware of what to watch for and report any concerns to your doctor or audiologist.
Use hearing assistance devices and services. Some of the negative effects of hearing loss can be prevented by using appropriate devices and services. Make sure you meet with the audiologist regularly and follow recommendations.
Protect your hearing. Everyday noise can damage hair cells of the inner ear. Loud sounds can damage hearing quickly, and even lower volumes can cause damage over time. Take care to limit exposure to loud sounds such as music, traffic, sporting events, and lawnmowers or construction equipment.
For parents: Understanding my child’s risk
Here is a quick list to help you talk to your doctor about risk for hearing loss. Children who receive cisplatin, carboplatin, or radiation to the head or neck should have hearing tested at least once after completion of treatment with follow-up testing as recommended.
Survivors of childhood cancer who have risk factors for hearing loss should have yearly check-ups with their primary doctor and make sure that hearing screens are part of regular follow-up care.
Additional resources on hearing loss