Diffuse Large B-Cell Lymphoma (DLBCL)
What is diffuse large B-cell lymphoma?
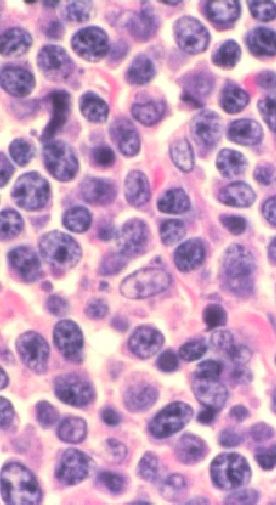
Diffuse large B-cell lymphoma (DLBCL) is a type of non-Hodgkin lymphoma. This disease starts in the B lymphocytes of the immune system. Normally, these cells fight infection and disease. But genetic changes in these cells can lead to cancer.
The abnormal lymphocytes grow larger and more quickly than normal cells. This disease can start in the lymph nodes or somewhere else in the body (known as an extranodal disease).
DLBCL grows fast and spreads quickly. The abnormal cells may travel through the lymphatic system. Because of this, DLBCL may develop in the:
- Lymph nodes
- Spleen
- Liver
- Bone marrow
- Gastrointestinal tract
- Brain
- Other organs
However, with early treatment, the 5-year survival rate is higher than 90% in the United States.
Symptoms of diffuse large B-cell lymphoma
Symptoms of DLBCL may include:
- Swollen lymph nodes in the neck, underarm, groin, or abdomen
- Fever
- Night sweats
- Weight loss
- Coughing
- Trouble breathing
- Swollen belly and/or belly pain
- Loss of appetite
- Nausea
- Vomiting
- Fatigue
Risk factors for diffuse large B-cell lymphoma
Risk factors may increase your child’s chances of getting a disease. Little is known about the risk factors for DLBCL in children. For lymphoma, the risk factors we know so far are:
- Weak immune system after a bone marrow or solid organ transplant
- Infection with Epstein-Barr virus or human immunodeficiency virus (HIV)
- A genetic disorder, such as ataxia-telangiectasia, that increases the risk of having cancer
- More common in males than females
- More common in White than Black children
Diagnosis of diffuse large B-cell lymphoma
A cancer diagnosis requires tests and procedures. The doctor will give your child a physical exam, ask about their medical history, and order tests such as:
See Waiting for Test Results.
If the pathologist finds lymphoma cells in the biopsy sample, the lab will do more lab tests on the sample, such as flow cytometry, immunophenotyping, and cytogenetic analysis, if they are available.
Types of diffuse large B-cell lymphoma
There are several types of DLBCL:
- Primary mediastinal B-cell lymphoma, which grows quickly in the chest
- CNS lymphoma, which grows in the central nervous system
- DLBCL-NOS, which has 2 types based on genetic changes:
- Germinal center B-cell (GBC; most common in children)
- Activated B-cell (ABC)
Your care team may order tests to find out which type of DLBCL your child has.
Stages of diffuse large B-cell lymphoma
The care team plans treatment based on the cancer stage. Some tumors grow rapidly. So, the doctor must stage the lymphoma as quickly as possible.
To find out the stage of disease, doctors may order more tests such as:
The stage will tell how much cancer is present and if it has spread to other parts of the body.
The International Pediatric Non-Hodgkin Lymphoma Staging System divides the disease into 4 stages:
- Stage 1 and 2 lymphomas are limited-stage disease and are treated the same way.
- Stage 3 and 4 lymphomas are advanced-stage disease. The treatment for both stages is similar, but the length of treatment may vary depending on the stage.
Treatment of diffuse large B-cell lymphoma
Treatment of DLBCL depends on:
- The type of lymphoma
- The stage of lymphoma
- How well the disease may respond to treatment
- Available treatments
- The patient’s age and health
Treatments may include:
Higher-stage, advanced disease is often treated with chemotherapy and immunotherapy. This is known as combination therapy. The most commonly used treatment in North America is the Lymphome Malin de Burkitt (LMB) treatment. It includes chemotherapy with or without the targeted therapy rituximab.
Treatment can sometimes cause side effects. One that may occur early in treatment is tumor lysis syndrome. This happens when cancer cells quickly die and break apart. The care team will watch your child closely for possible side effects. Ask the care team if you have questions.
Relapsed disease
A common chemotherapy plan for relapsed disease is RICE (rituximab, ifosfamide, carboplatin, and etoposide) followed by a stem cell transplant. New targeted therapies are being studied. Some patients may be able to take part in clinical trials to test new treatments.
Prognosis for diffuse large B-cell lymphoma
The prognosis depends on several factors, including the stage of the disease.
In the United States, the 5-year survival rate for limited-stage (stage 1 and 2) diffuse large B-cell lymphomas is higher than 95%. The survival rate for advanced-stage (stage 3 and 4) DLBCL is higher than 90%.
Support for patients with diffuse large B-cell lymphoma
Coping with a cancer diagnosis and treatment can be stressful for the patient and the family. Talking to a social worker, psychologist, or another mental health specialist may help.
Learn how to talk to your child about cancer.
After treatment, your care team may use imaging tests and exams to watch for recurrence.
Childhood cancer survivors should get follow-up care throughout their lives. Some treatments can cause late effects. These are health problems that happen months or years after treatment ends.
After completing treatment, it is important that your child:
- Has regular checkups and screenings by a primary care provider
- Maintains healthy habits to protect their health, including physical activity and healthy eating
- Has a survivorship care plan to share with their health providers, which includes:
- Guidance on health screenings
- Disease risk factors
- Ways to improve health
Questions to ask your care team
- What does the biopsy show?
- What stage of cancer does my child have?
- What are my child’s treatment options?
- What are the possible side effects of each treatment?
- How can my child manage their side effects?
- Will my child need to be in the hospital for treatment?
- Where is the treatment available? Is it close to home or will we have to travel?
- What resources are available to help us cope with this illness?
- What monitoring does my child need after treatment?
- How can I help my child stay healthy?
- What are the possible late effects of treatment?
Key points about diffuse large B-cell lymphoma
- Diffuse large B-cell lymphoma (DLBCL) is a form of non-Hodgkin lymphoma that affects B lymphocytes.
- Doctors diagnose this cancer using a physical exam, blood tests, imaging, and biopsy.
- Treatment options may include chemotherapy, combination therapy, stem cell therapy, targeted therapy, radiation therapy, surgery, or immunotherapy.
- Treatment depends on the type of DLBCL, genetic changes, stage of disease, the patient’s health, and available therapies.
- The overall 5-year survival rate is higher than 90% depending on the stage at diagnosis. Every case is different. Your doctor is the best source of information about your child’s case.
Find out more information
-
Lymphoma
Lymphoma is a cancer of the lymphatic system, which is a network of nodes, glands, and vessels that transports lymphocytes throughout the body.
-
Non-Hodgkin Lymphoma
Non-Hodgkin lymphoma is a cancer of the lymphatic system. There are about 800 new cases diagnosed in U.S. children and teens each year.
-
Basics of Blood
Learn about what blood is and how it functions including healthy blood formation, cancers of the blood, and treatment.