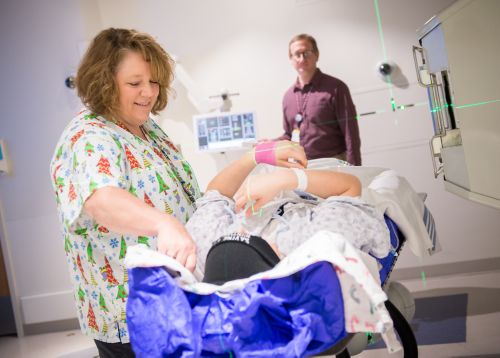
Helping your child stay still during radiation simulation
A device may be made to help your child stay still during treatment. If a device is made, it will be used for each treatment.
Mask
The therapist may use a mask to hold your child’s head in the correct position. This mask is made from a flat piece of plastic that has small holes in it. It is made just for your child.
To make the mask, the therapist will:
- Help your child get into the correct position.
- Place a flat, plastic sheet in a dry heat oven to make it soft.
- Take the plastic out of the oven for a few seconds so it can cool.
- Place the plastic on your child’s face and stretch it down over the chin.
As it cools, the plastic hardens. Your child will be able to breathe easily through holes in the mask.
If your child’s treatment requires a mask, their hair should be in the same style for each simulation and treatment. Sometimes, the care team may ask that your child get a haircut before their session. This helps make sure the mask holds your child’s head in the correct position.
Headrest
The therapist may make a mold that supports your child’s head while they are lying on their back. To make this mold, the therapist will:
- Help your child get into the correct position.
- Place a flat, plastic sheet in a dry heat oven to make it soft.
- Take the plastic out of the oven for a few seconds so it can cool.
- Place the plastic under your child’s head.
As it cools, the plastic hardens. The mold forms into the shape of the back of your child’s head
If your child will be on their stomach during treatment, a similar facemask will be made. The therapist will place an oxygen tube between the table and the mask so your child can breathe easily.
Vac lock bag
A vac lock bag is a type of body mold that helps hold your child’s body in the correct position. It can support the head, abdomen, leg, or another part of the body. Your child will lie on the bag. A vacuum will remove the air from the bag, causing the bag to mold around your child’s body.
Alpha cradle
An alpha cradle is used for Total Body Irradiation (TBI). To create an alpha cradle:
- Your child will lie on the TBI table, on top of a vac lock bag.
- The therapist will pour a foaming solution inside a plastic bag (the alpha cradle).
- The therapist will place the bag on top of your child like a blanket.
- The bag will harden and form the shape of your child’s body.
General anesthesia
Your child may need general anesthesia to help them stay still during the radiation treatment. Your medical team will discuss this with you. In some cases, your care team may recommend that your child try the simulation without anesthesia.
If your child gets anesthesia, you or another caregiver may stay with them until they fall asleep. The anesthesia team monitors your child the whole time. They will call you to the recovery room when your child wakes up.
Your care team will let you know your schedule for simulation and radiation treatments. Your child may also have an appointment with a child life specialist. If you have questions about simulation or radiation therapy, talk to your care team.